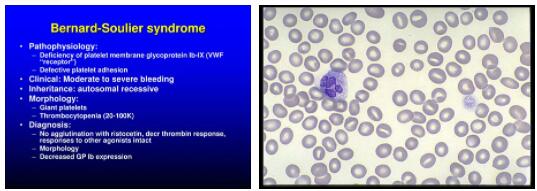
The Bernard-Soulier syndrome, also known as Hemorrhagic Thrombozytendystrophie or BSS known is an extremely rare bleeding disorder. BSS is inherited as an autosomal recessive trait. The syndrome itself is counted among the so-called thrombocytopathies. So far, just one hundred cases have been documented; however, the course of the disease is positive.
What is Bernard Soulier Syndrome?
Abbreviated as BSS by AbbreviationFinder.org, the Bernard-Soulier syndrome – also called BSS for short – is an autosomal recessive hereditary bleeding disorder, which is a hereditary thrombocytopathy. BSS is also often referred to as giant platelet syndrome ; In addition to bleeding, people with BSS experience extremely enlarged platelets.
The name – Bernard Soulier Syndrome – comes from two French hematologists. Jean-Pierre Soulier and Jean-Bernard discovered the syndrome and wrote the first notes as early as 1948, which sometimes describe the symptoms of Bernard Soulier syndrome. This is mainly the talk of the giant platelets and prolonged bleeding.
Causes
The BSS is a form of platelet dystrophy. It is not known at what age the first symptoms appear. There are always different information; Furthermore, so few people are affected by Bernard Soulier Syndrome that there are around one hundred cases that have actually been documented. The cause of the Bernard Soulier syndrome is a platelet adhesion disorder.
This is an inheritable defect in a so-called membrane receptor, which subsequently triggers the syndrome. For this reason, doctors speak of a point mutation, which can also be referred to as a nonsense mutation. The mutation is on the glycoprotein Ib or the coding GPIb. However, the disorders of the platelet functionality cause the bleeding. This disrupts or prevents the platelets from clumping together.
That approach arises from the fact that the necessary receptors have a lack of blood clotting. However, there are 30 known or different mutations of the so-called glycoproteins that subsequently trigger the Bernard-Soulier syndrome. However, all forms have in common the fact that there is platelet dysfunction.
Symptoms, ailments & signs
Classic symptoms are hemorrhagic diathesis and a tendency to bruise. In the case of hemorrhagic diathesis, the doctor describes an extremely strong tendency to bleed. Bleeding can occur so heavily and for a long time for no particular reason. For this reason, the treatment focuses on reacting in advance to any blood loss (e.g. during operations).
As a result, hematomas naturally form relatively quickly. Other symptoms and features that are characteristic of Bernard Soulier syndrome: nosebleeds, purpura, gastrointestinal bleeding as well as spontaneous bleeding (mainly on the mucous membranes) and significantly prolonged menstrual bleeding in women.
Diagnosis & course of disease
The doctor makes the diagnosis of Bernard Soulier syndrome as part of the anamnesis, the blood values from the laboratory and a visual finding. For the doctor, for example, it is important how often hematomas form or how often the affected person bleeds for no reason and how long the bleeding lasts. A blood smear is taken from the person concerned for the laboratory.
The doctor mainly makes sure that he is concentrating on the macrothrombocytosis. These are those giant platelets that sometimes provide a certainty that the person affected actually suffers from Bernard Soulier syndrome. Experts also check the number of blood platelets as part of the complete blood count. Those affected show a significantly reduced number here. Individuals with Bernard Soulier Syndrome have fewer than 30,000 platelets (measured per microliter); the normal value is between 150,000 and 400,000 platelets.
The size of the platelets is between four and 10 micrometers; However, normal or healthy platelets are only one to a maximum of four micrometers in size. Furthermore, the person concerned also finds that the duration of the bleeding doubles again and again. Another reason that the medical professional can be sure that it is Bernard-Soulier syndrome.
The attending physician obtains confirmation of his suspected diagnosis by means of coagulation diagnostics. However, if one considers all cases of illness and their course of illness, one can assume that the prognosis is favorable.
Complications
In most cases, Bernard-Soulier syndrome can be treated relatively well, so that there are no further complications for the patient. The patient has increased bleeding, which in many cases is difficult to stop. For this reason, in the event of an accident or surgery, care must always be taken to take Bernard-Soulier syndrome into account and, if necessary, to stop the bleeding.
Often there is an unexpected nosebleed or bleeding in the gastrointestinal area. Women also suffer from long and heavier menstrual periods due to Bernard-Soulier syndrome. The patient is restricted in his everyday life by the heavy bleeding. As a rule, there are no particular complications if the bleeding is treated correctly and stopped in a timely manner.
A causal treatment is not possible in the case of Bernard Soulier syndrome, as the syndrome is still largely unexplored. If there is severe blood loss, this must be compensated for. The bleeding can also be restricted with the help of medication.
Bernard-Soulier syndrome usually does not reduce the patient’s life expectancy. However, doctors must be informed if the Bernard-Soulier syndrome is present, as otherwise severe and unexpected bleeding can occur during surgical interventions.
When should you go to the doctor?
In the case of Bernard Soulier syndrome, a doctor must be consulted in any case. In this way, complaints and other complications can be significantly reduced, which also significantly increases the life expectancy of the person affected. As a rule, in the case of Bernard Soulier syndrome, a doctor must be consulted if the person concerned detects an increased tendency to bleed. The bleeding can also occur spontaneously. Even small injuries or cuts lead to profuse bleeding that cannot be stopped easily.
In acute emergencies, an emergency doctor must be called or a hospital visited. However, the doctor must be informed about the Bernard-Soulier syndrome before a surgical procedure so that this bleeding can be avoided directly. Frequent nosebleeds or spontaneous bleeding in women also indicate Bernard-Soulier syndrome, so that an examination should be carried out by a doctor.
The diagnosis of Bernard Soulier syndrome can be made by a general practitioner. The syndrome can be identified through a blood test. Treatment itself is carried out with the help of drugs. Doctors should be warned about surgical procedures to avoid complications.
Treatment & Therapy
Doctors usually aim for symptomatic therapy. This means that doctors cannot treat the cause, but primarily only the symptoms. In certain cases, medical professionals will also intervene directly in the patient’s organism using platelet concentrates. However, these acute cases and interventions only occur when large blood losses are already possible or imminent.
For example, before surgical interventions. Here the patient is given so-called platelet transfusions. Otherwise, doctors try to design the therapy in such a way that primarily the organism is spared. Sometimes the doctors intervene using special medication, even if it is an intraoperative measure.
Further treatment can sometimes take place intrapartally or prepartally. This means that therapies are carried out before the birth. Occasionally, however, it happens again and again that there is longer and heavier bleeding here too. Above all, menstrual bleeding (menstrual bleeding) and injuries are classic examples of why those affected bleed longer and more heavily.
Outlook & forecast
There is no prospect of a cure for Bernard Soulier syndrome. The disease is based on a genetic defect that cannot be repaired with the existing medical and therapeutic options. In addition, interference and changes in human genetics are not permitted for legal reasons. Therefore, the disease has so far been considered incurable.
In medical care, the doctors concentrate on alleviating the symptoms. This works very well with most patients. The platelet concentration in the blood is measured at regular check-ups. If it is too low, a blood transfusion increases the number of platelets.
This process is routine and completed within one treatment. However, since this method is not sustainable, regular transfusions are used. Without using the transfusion, there is a risk that the patient will experience profuse bleeding that cannot be stopped. In severe cases, there is a risk of severe blood loss, which without medical care can be fatal.
As a precaution, people with Bernard Soulier syndrome should be given sufficient blood transfusions before surgery. If you lose too much blood during an operation because the bleeding cannot be stopped, you are at an increased risk of complications. Overall, sick people can achieve a good quality of life with the disease by avoiding risky situations.
Prevention
There is no prevention. Since the Bernard-Soulier syndrome is hereditary, no measures can be taken to prevent the Bernard-Soulier syndrome. So far, however, only around 100 cases have been documented; the likelihood of developing Bernard Soulier syndrome is therefore extremely low or very unlikely.
Aftercare
The hereditary Bernard-Soulier syndrome (BSS) is characterized by a platelet dysfunction. This requires permanent treatment as it can easily lead to bleeding. In diseases such as hemorrhagic platelet dystrophy, coagulation disorders are present.
These can show up through frequent bruising or a tendency to bleed, even for trivial reasons. Due to the nature of the disease, acute treatment and aftercare usually merge into one another. Thanks to the hereditary component of Bernard Soulier syndrome, there is no cure for the symptoms.
Follow-up care is so important because the patient must avoid mistakes that increase the tendency to bleed. For example, he is not allowed to take acetylsalicylic acid preparations and pain relievers. He should also avoid foods like garlic. These thin the blood and can increase the risk of bleeding. Follow-up care after the diagnosis should therefore also include nutritional advice.
The risk of bleeding when diagnosed with Bernard Soulier syndrome increases if the body is subjected to blunt violence or accidental trauma. In the worst case, such effects can lead to massive blood loss and a subsequent hypovolemic shock. Those affected must therefore ensure that the emergency doctors are immediately informed of the presence of Bernard Soulier syndrome.
In comparison with other blood diseases of a similar kind, there is no immediate danger to life for people with Bernard-Soulier syndrome. In the event of severe bleeding after an accident, platelet preparations can be administered.
You can do that yourself
Since the Bernard-Soulier syndrome has been shown to be based on a genetic defect, there is no prospect of a cure. Nevertheless, those affected who receive medical care manage to achieve a good quality of life and a normal life expectancy.
It is important to have the concentration of platelets in the blood measured during regular check-ups. If this is too low, it is increased with the help of blood transfusions. Patients should also receive transfusions before upcoming operations or delivery to avoid complications.
In everyday life it is important to avoid risky situations. Extreme sports are strongly discouraged as they pose a high risk of injury. But team and contact sports always carry the risk of minor and major injuries, which can quickly lead to excessive bleeding in those affected.
For women who suffer from increased menstrual bleeding due to the disease, the market offers sufficiently strong and safe hygiene products in different strengths.
Above all else, regular medical and laboratory examinations are the key to less stressful handling of Bernard Soulier syndrome in everyday life. Patients who receive good therapeutic care can, however, go about their everyday life normally with these restrictions and rules of conduct.