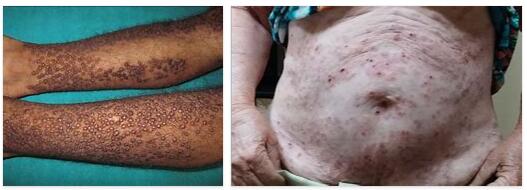
A bullous pemphigoid is an autoimmune disease of the skin, accompanied by bubble formation and its incidence from age 60 significantly increases. With around 0.7 to 1.8 new cases per 100,000 inhabitants annually, bullous pemphigoid is a rare disease, although it is the most common autoimmune blistering dermatosis.
What is a bullous pemphigoid?
Bullous pemphigoid is an autoimmune skin disease (autoimmune dermatosis) associated with subepidermal, bulging blisters (bullae).
The not infrequently hemorrhagic (leading to bleeding) blisters can manifest themselves on reddened (on erythema) and healthy skin. In particular, the abdomen and intertrigines (including armpits, flexors of the extremities, groin region, gluteal folds) are affected by blistering, while the oral mucosa is usually not involved (around 20 percent).
Bullous pemphigoid is often associated with certain autoimmune diseases such as ulcerative colitis, polymyositis or chronic polyarthritis and, in rare cases, with malignant tumors. In addition to the firm, firm blisters, which are the main symptom of bullous pemphigoid and in some cases can be announced by itching or wheals (urticaria), pyoderma (purulent inflammation of the skin) can develop as a result of a secondary streptococcal or staphylococcal infection.
Causes
The bullous pemphigoid is an autoimmune disease and is accordingly due to a dysregulation of the immune system. The body’s own autoantibodies, so-called immunoglobulins G (IgG), are formed by the immune system, which are directed against certain proteins of the hemidesmosomes, which, as cellular components of the cell membrane, ensure the connection between the epidermis and the basement membrane (between the epidermis and the dermis or the dermis) are.
Macrophages (scavenger cells) and monocytes (precursor of macrophages) destroy the areas of the hemidesmosomes that the autoantibodies mistakenly mark as pernicious (malignant), so that the adhesion (cohesion) between the affected skin layers is no longer guaranteed. Fluid build-up occurs, causing blisters to form.
Exactly what causes this incorrect regulation has not been clearly clarified. It is known that bullous pemphigoid can be triggered (triggered) by drugs such as furosemide, diazepam, diuretics or ACE inhibitors, certain malignant tumors (including bronchial and prostate carcinoma) and UV radiation.
Symptoms, ailments & signs
Bullous pemphigoid manifests itself primarily through the noticeable changes in the skin. Most people develop redness and reddened nodules, some of which are swollen and very itchy. After weeks or months, these bumps develop into small vesicles. These can appear on reddened skin, but often also spread to healthy areas of the skin.
Usually they are a few millimeters to two centimeters in size and filled with a clear, yellowish liquid. Occasionally the bladders are partially filled with blood. The top of the blisters is formed by the epidermis, which is why a bullous pemphigoid is usually very resistant and plump.
If it opens, superficial, easily bleeding and oozing skin defects appear on the affected area. Redness, swellings, lumps and skin defects often coexist and form the complexion that is characteristic of the disease. The skin changes can occur anywhere on the body.
They are particularly common on the abdomen, armpits, groin, inner thighs, and the hips of the arms. The oral mucosa or the conjunctiva are affected in every fifth patient. The painful erosions occur in bursts and often heal on their own. In the absence of treatment, a bullous pemphigoid can last for years.
Diagnosis & course
Bullous pemphigoid can usually (about 80 to 90 percent) in addition to the main clinical symptom (bulging blisters) on the basis of the detection of autoantibodies (IgG and its complement C3) against hemidesmosomes in the lamina lucida of the basement membrane (direct immunofluorescence) or in the serum (indirect immunofluorescence) can be diagnosed by fluorescent anti-antibodies.
In addition, in some cases the sedimentation rate is increased and peripheral eosinophilia (increased concentration of eosinophilic granulocytes) or other immunoglobulins (IgE) can be detected in the serum. Histologically (fine tissue) infiltrates of the dermis can be detected by eosinophils and neutrophils (certain leukocytes) as well as lymphocytes and histiocytes.
With the help of imaging procedures (chest x-ray, abdominal sonography) and a blood stool, tumors can be excluded as triggers. Bullous pemphigoid develops spontaneously in most cases and has a relapsing, relapsing course. If untreated, a bullous pemphigoid is fatal in 30 to 40 percent of cases.
Complications
As a rule, the bullous pemphigoid significantly limits the patient’s quality of life. There are strong and very unpleasant discomforts on the skin of the person concerned. Itching develops, which is associated with reddening of the skin. If the patient scratches the skin, the itching tends to get worse.
The loss of appetite that occurs also leads to a significant loss of weight and thus often to underweight. This makes the patient feel weakened. There is also a high fever. The treatment itself is carried out with the help of antibiotics and immunosuppressants. These can lead to minor side effects, which, however, depend on the patient’s state of health.
In most cases, taking the medicine leads to a positive course of the disease. However, the person affected can develop the disease again later in life. If drug treatment is unsuccessful, immunoglobulins can be administered intravenously.
As a rule, this leads to a positive course of the disease. There are no further complications. The life expectancy of the patient is not changed either.
When should you go to the doctor?
If itching, reddening of the skin, or the characteristic blisters are noticed, a doctor should be informed. It is best to consult a doctor quickly, especially if the symptoms increase. This is especially true when the symptoms have a significant impact on wellbeing.
It is advisable to have a possible bullous pemphigoid clarified quickly before further complications arise. Anyone who notices physical exhaustion in a relative and sometimes also isolation from social contacts should speak to them immediately.
With support, the visit to the doctor and the subsequent treatment are often easier. The skin disease occurs predominantly in older people – in addition to the recommended routine examinations, a doctor should be consulted immediately in the event of unusual symptoms. If a bullous pemphigoid is found, it can usually be treated well.
Since drug therapy involves certain risks, the following applies: Consult your doctor regularly. If there are severe side effects, an appointment should be made with the family doctor. Other contact persons are the dermatologist or – in the case of severe complaints – the medical emergency service.
Treatment & Therapy
In the case of bullous pemphigoid, therapy consists of topical or local as well as systemic treatment measures and aims at immunosuppression through a drug-based reduction in autoantibody synthesis using immunosuppressants or steroids.
The therapeutic measures depend on the extent of the disease, the age and the underlying diseases of the specific person affected as well as the extent (locally limited or generalized) and the trigger of the skin disease. If the pemphigoid is induced by drugs, for example, the triggering substances must be discontinued or changed accordingly.
In the case of a mildly bullous pemphigoid, an effective topical glucocorticoid or steroid is sufficient for treatment in many cases. This is applied to the affected skin areas in combination with antiseptic ointments or creams such as clioquinol cream, ethacridine lactate ointment and cadexomer iodine.
As a rule, the blisters are opened and punctured prior to topical treatment. For systemic or internal treatment of moderate bullous pemhigoids, oral or intravenous infused glucocorticoids are also used, which are combined with azathioprine and the dose of which is gradually (gradually) reduced over the course of therapy.
Oral application of niacinamide (nicotinic acid amide) and tetracycline in combination with topical glucocorticoids are just as successful, although such a therapy acts on the local inflammation mediators and does not inhibit the formation of antibodies. In isolated cases, high-dose corticosteroids, intravenously infused immunoglobulins or plasmapheresis are used, which is usually not necessary in the case of a common bullous pemphigoid.
Outlook & forecast
Most patients with this disease are dependent on lifelong therapy because the cause of the disease cannot be treated. If the disease occurs through various triggering substances, these must be discontinued in order to alleviate the symptoms.
Typically, patients rely on medication and various creams and ointments to improve their quality of life and manage symptoms. The exact treatment depends heavily on the severity of the symptoms. There are no particular complications with the treatment and the symptoms are alleviated.
If the disease is not treated, the symptoms remain and have a very negative effect on the patient’s quality of life and everyday life. This not only results in restrictions in everyday life, but often also in psychological complaints or the development of depression. For this reason, treatment is necessary in every case. The life expectancy of the patient is not limited by the disease. In some cases the symptoms go away with old age, although this course is not yet fully understood.
Prevention
Since the exact triggers for a manifestation of bullous pemphigoid have not been conclusively clarified, it cannot be prevented directly. Known potential factors that can promote the development of pemphigoid (including medication) should be avoided if necessary.
Aftercare
In most cases, there are no special or direct measures and options for follow-up care available to the person affected. The person concerned is therefore primarily dependent on a quick and above all on an early diagnosis and treatment of this disease, so that further complications can be prevented. Self-healing cannot occur, so treatment is absolutely necessary.
The treatment itself is usually done with the help of medication. These should be taken regularly and in the correct dosage to prevent further complications. If you have any questions or are unclear, you should always contact a doctor first so that no further complaints arise. Unfortunately, most people affected by this disease are also dependent on dialysis.
In doing so, they often need the support and care of friends and family. Sensitive and loving conversations are also necessary so that there are no psychological upsets or depression. Whether the disease will lead to a reduction in life expectancy cannot be universally predicted. Further follow-up measures are not possible.
You can do that yourself
Bullous pemphigoid is a rare autoimmune skin disorder that affects people over the age of 60 in particular. The causes have not yet been conclusively clarified, but a connection between the disease and certain drugs, for example diuretics or ACE inhibitors, is suspected.
If patients notice symptoms of the disease, it is imperative that they consult a doctor or specialist clinic specializing in autoimmune diseases as soon as possible and inform their contact person about the medication they are taking.
The patients usually suffer from very severe itching, which is usually treated by a doctor. Antihistamines, which are available as ointments, tablets or drops in the pharmacy without a prescription, also help on vacation or in other exceptional situations. The itching often increases when it is warm. Many patients suffer from particularly severe itching under the duvet, especially at night.
Here it can help to replace conventional duvets with light polar fleece duvets. These textiles are very light and breathable, so that there is no heat build-up. If you have blisters on your body, you should wear loose-fitting clothing and underwear with a high proportion of breathable materials such as cotton or bamboo.
If there are blisters on parts of the body that cannot be covered with clothing, these skin changes often have a disfiguring effect. The bubbles can be optically concealed with the help of special make-up from the pharmacy or cosmetic retailer.